 Sometimes collaterals from vein occlusions can look like IRMAs. The above assumes screen settings, colour balance, monitor, software and camera settings are optimal according to the recommendations of the NHS DES Programme. If an IRMA can only be seen on a red free image and not on the colour image a referral should not be made (returned to annual screening). IRMA is considered present if the IRMA can still be seen on the colour image, that has not been enlarged, as well as on the red free. If an IRMA is found, the grader should return to the colour image. Only IRMAs that are definitely seen should be classified as R2. MBH nasal 2.5 Intraretinal microvascular abnormality ( IRMA) Any haemorrhage that is flame shaped or any MA should not be counted as a blot. This is provided the veins are not very dilated.įlame haemorrhages are superficial haemorrhages in the nerve fibre layer. Blot haemorrhages are larger than the width of the smallest of the 4 branches of the central retinal vein as it crosses the edge of the disc. The difference between a dot and a blot is one of size. They are restricted in a particular location, and so take longer to clear than a superficial haemorrhage. These haemorrhages are in the retina’s inner nuclear and outer plexiform layers. Most experts grade the MBH image set as having between 8 and 10 blot haemorrhages across both images. The difficulties of counting blot haemorrhages are recognised. An image which has this number of blot haemorrhages, or more, is referable. The MBH (previously known as MBH 3) images below shows the amount of haemorrhage present in the retina to warrant an R2 classification. If uncertain, refer only in the presence of IRMA that are definitely seen. Venous beading from ischaemia in DR does not take place in isolation from MBH or IRMA. IRMA (check that they can still be seen on a colour image which has not been enlarged).multiple blot haemorrhages ( MBH) (refer only in the presence of IRMA that are definitely seen if uncertain).venous beading (venous beading from ischaemia in DR does not occur in isolation).Grading classification for pre‐proliferative DR (R2) The radius is the distance between the centre of the fovea and the temporal margin of the disc. The macula is defined as the part of the retina which lies within a circle centred on the centre of the fovea. Assign a P1 grade if evidence of previous photocoagulation (focal/grid to macula or peripheral scatter). 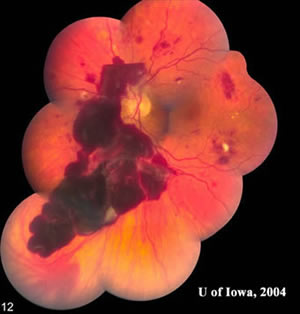
1.5 Photocoagulation scarsĪssign a P0 grade if no evidence of previous photocoagulation. 1.4 Venous loopsĪ venous loop should no longer be referred and should be regarded as a feature of R1. 
Where CWS are detected, graders should ensure they have checked for features of referable DR – in particular IRMA and early venous beading. Isolated cotton wool spots (one or more) in the absence of any microaneurysm or haemorrhage should be counted as no DR (R0).Īny number of cotton wool spots ( CWS) in the presence of other non‐referable features of DR should be graded as background DR (R1). Intraretinal microvascular abnormality ( IRMA) should not be recorded unless visible on colour images, without enlarging the image area, in addition to red free images. Microaneurysms should be differentiated from pigment spots by viewing in colour and red free and from artefacts by viewing on overlapping images where possible. This includes:Īvoiding excessive enhancement of images (beyond scale of 1:1) Equipment should meet national specifications and used in line with recognised procedures for grading. Grading should be carried out in accordance with national guidance. There are FBG forms for routine digital screening, digital surveillance (DS) and slit lamp biomicroscopy (SLB) surveillance. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
